CARING FOR PATIENT With PERIPHERAL VASCULAR DISORDERS
TERMINOLOGIES: use the link below to listen to how the terms are pronounced http://www.oddcast.com/home/demos/tts/tts_example.php
- Phlebotomy
- Venipuncture
- Syringe
- Needle
- Vacuum
- Vacuum tube
- Tourniquet
- Additives
- Central line
- Bacteremia
- Fungemia
- Air embolism
- IV : INTRAVENOUS
Risk factors for peripheral vascular disease include elevated blood cholesterol, diabetes, smoking, hypertension, inactivity, overweight and obesity
COMMON DISORDERS OF PERIPHERAL VASCULAR SYSTEM
- spider and varicose veins
- Deep vein Thrombosis
INTRODUCTION
Vascular disorder is a form of cardiovascular disease primarily affecting the blood vessels
Blood vessels mainly are arteries and veins. Vascular disease is a pathological state of large and medium sized muscular arteries and is triggered by endothelial cell dysfunction. Because of factors like pathogens, oxidized LDL particles and other inflammatory stimuli endothelial cells become activated. This leads to change in their characteristics:
Endothelial cells start to excrete cytokines and chemokine’s and express adhesion molecules on their surface. This in turn results in recruitment of white blood cells (monocytes and lymphocytes), which can infiltrate the blood vessel wall. Stimulation of smooth muscle cell layer with cytokines produced by endothelial cells and recruited white blood cells causes smooth muscle cells to proliferate and migrate towards the blood vessel lumen. The process causes thickening of the vessel wall, forming a plaque consisting of proliferating smooth muscle cells, macrophages and various types of lymphocytes. This plaque result in obstructed blood flow leading to diminished amounts of oxygen and nutrients that reaches the target organ.
The blood vessels are also responsible for transport of blood, nutrients and oxygen to target organs.
Diagnosis for affection of vascular system is either Invasive (angiography) or Noninvasive (ultrasound..etc.)
For the diagnosis and treatment blood sample are also taking from the vessels it is necessary to know and learn techniques used for effective blood sample taking
Also fluids and drugs are administered through the blood vessels and caution should be taken in setting IV access and lines
DISORDER OF PERIPHERAL VASCULAR SYSTEM
ATHEROSCLEROSIS; these is peripheral artery occlusive disease in which blood flow is restricted in the arteries due to build up of plaque inside the lumen of the artery and as a result less oxygen and nutrients are delivered to the tissue of the body.
Plaque is an injury on the endothelium or inner lining of the artery and can cause blood clot to form as response to injury. This clot can sometimes break off and become emboli which can travel and plug distant vessels.
the plaque changes the elasticity of the arterial wall and make the artery brittle and inelastic. the arteries affected are more prone to breaking or rupture.
depending on the affected artery the following complication can develop from atherosclerosis
- atherosclerosis of brain arteries can cause stroke
- atherosclerosis of coronary arteries of the heart can cause myocardial infarction
- atherosclerosis of the renal arteries can cause renal renal failure
- atherosclerosis of the arteries supplying the leg can cause peripheral vascular disease, which initial symptom is intermittent claudication
The cause of atherosclerosis isn’t known. However, certain traits, conditions, or habits may raise your risk for the disease. These conditions are known as risk factors.
You can control some risk factors, such as lack of physical activity, smoking, and an unhealthy diet. Others you can’t control, such as age and a family history of heart disease.
Some people who have atherosclerosis have no signs or symptoms. They may not be diagnosed until after a heart attack or stroke.
The main treatment for atherosclerosis is lifestyle changes. You also may need medicines and medical procedures. These treatments, along with ongoing medical care, can help you live a healthier life.
diagnosis for atherosclerosis;
- physical examination
- Diagnostic tests: Blood tests check the levels of certain fats, cholesterol, sugar, and proteins in your blood. Abnormal levels may be a sign that you’re at risk for atherosclerosis.
- An EKG is a simple, painless test that detects and records the heart’s electrical activity. The test shows how fast the heart is beating and its rhythm (steady or irregular). An EKG also records the strength and timing of electrical signals as they pass through the heart.
- Angiography (an-jee-OG-ra-fee) is a test that uses dye and special x rays to show the inside of your arteries. This test can show whether plaque is blocking your arteries and how severe the blockage is.A thin, flexible tube called a catheter is put into a blood vessel in your arm, groin (upper thigh), or neck. Dye that can be seen on an x-ray picture is injected through the catheter into the arteries. By looking at the x-ray picture, your doctor can see the flow of blood through your arteries.
Living With Atherosclerosis
Improved treatments have reduced the number of deaths from atherosclerosis-related diseases. These treatments also have improved the quality of life for people who have these diseases.
Adopting a healthy lifestyle may help you prevent or delay atherosclerosis and the problems it can cause. This, along with ongoing medical care, can help you avoid the problems of atherosclerosis and live a long, healthy life.
Researchers continue to look for ways to improve the health of people who have atherosclerosis or may develop it.
Ongoing Care
If you have atherosclerosis, work closely with your doctor and other health care providers to avoid serious problems, such as heart attack and stroke.
Follow your treatment plan and take all of your medicines as your doctor prescribes. Your doctor will let you know how often you should schedule office visits or blood tests. Be sure to let your doctor know if you have new or worsening symptoms.
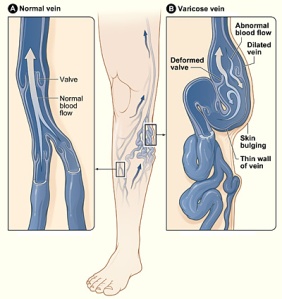
VARICOSE VEIN;
Varicose (VAR-i-kos) veins are swollen, twisted veins that you can see just under the surface of the skin. These veins usually occur in the legs, but they also can form in other parts of the body.
Varicose veins are a common condition. They usually cause few signs and symptoms. Sometimes varicose veins cause mild to moderate pain, blood clots, skin ulcers (sores), or other problems.
Overview
Veins are blood vessels that carry blood from your body’s tissues to your heart. Your heart pumps the blood to your lungs to pick up oxygen. The oxygen-rich blood then is pumped to your body through blood vessels called arteries.
From your arteries, the blood flows through tiny blood vessels called capillaries, where it gives up its oxygen to the body’s tissues. Your blood then returns to your heart through your veins to pick up more oxygen.
Veins have one-way valves that help keep blood flowing toward your heart. If the valves are weak or damaged, blood can back up and pool in your veins. This causes the veins to swell, which can lead to varicose veins.
Many factors can raise your risk for varicose veins. Examples of these factors include family history, older age, gender, pregnancy, overweight or obesity, and lack of movement.
Varicose veins are treated with lifestyle changes and medical procedures. The goals of treatment are to relieve symptoms, prevent complications, and improve appearance.Sometimes varicose veins cause pain, blood clots, skin ulcers, or other problems
What Causes Varicose Veins?
Weak or damaged valves in the veins can cause varicose veins. After your arteries and capillaries deliver oxygen-rich blood to your body, your veins return the blood to your heart. The veins in your legs must work against gravity to do this.
One-way valves inside the veins open to let blood flow through, and then they shut to keep blood from flowing backward. If the valves are weak or damaged, blood can back up and pool in your veins. This causes the veins to swell.
Weak vein walls may cause weak valves. Normally, the walls of the veins are elastic (stretchy). If these walls become weak, they lose their normal elasticity. They become like an overstretched rubber band. This makes the walls of the veins longer and wider, and it causes the flaps of the valves to separate.
When the valve flaps separate, blood can flow backward through the valves. The backflow of blood fills the veins and stretches the walls even more. As a result, the veins get bigger, swell, and often twist as they try to squeeze into their normal space.
How Are Varicose Veins Diagnosed?
- physical examination
- Doppler ultrasound; During this test, a handheld device will be placed on your body and passed back and forth over the affected area. The device sends and receives sound waves. A computer will convert the sound waves into a picture of the blood flow in your arteries and veins.
- Angiogram
Varicose veins are treated with lifestyle changes and medical procedures. The goals of treatment are to relieve symptoms, prevent complications, and improve appearance.
Lifestyle Changes
Lifestyle changes often are the first treatment for varicose veins. These changes can prevent varicose veins from getting worse, reduce pain, and delay other varicose veins from forming. Lifestyle changes include the following:
- Avoid standing or sitting for long periods without taking a break. When sitting, avoid crossing your legs. Keep your legs raised when sitting, resting, or sleeping. When you can, raise your legs above the level of your heart.
- Do physical activities to get your legs moving and improve muscle tone. This helps blood move through your veins.
- If you’re overweight or obese, try to lose weight. This will improve blood flow and ease the pressure on your veins.
- Avoid wearing tight clothes, especially those that are tight around your waist, groin (upper thighs), and legs. Tight clothes can make varicose veins worse.
- Avoid wearing high heels for long periods. Lower heeled shoes can help tone your calf muscles. Toned muscles help blood move through the veins.
compression stockings These stockings create gentle pressure up the leg. This pressure keeps blood from pooling and decreases swelling in the legs.
There are three types of compression stockings.
One type is support pantyhose; These offer the least amount of pressure.
A second type is over-the-counter compression hose; These stockings give a little more pressure than support pantyhose. Over-the-counter compression hose are sold in medical supply stores and pharmacies.
Prescription-strength compression hose are the third type of compression stockings. These stockings offer the greatest amount of pressure. They also are sold in medical supply stores and pharmacies
Medical Procedures
Medical procedures are done either to remove varicose veins or to close them. Removing or closing varicose veins usually doesn’t cause problems with blood flow because the blood starts moving through other veins.
You may be treated with one or more of the procedures described below. Common side effects right after most of these procedures include bruising, swelling, skin discoloration, and slight pain.
The side effects are most severe with vein stripping and ligation (li-GA-shun). Rarely, this procedure can cause severe pain, infections, blood clots, and scarring.
Sclerotherapy
Sclerotherapy (SKLER-o-ther-ah-pe) uses a liquid chemical to close off a varicose vein. The chemical is injected into the vein to cause irritation and scarring inside the vein. The irritation and scarring cause the vein to close off, and it fades away.
This procedure often is used to treat smaller varicose veins and spider veins. It can be done in your doctor’s office, while you stand. You may need several treatments to completely close off a vein.
Treatments typically are done every 4 to 6 weeks. Following treatments, your legs will be wrapped in elastic bandaging to help with healing and decrease swelling.
Microsclerotherapy
Microsclerotherapy (MI-kro-SKLER-o-ther-ah-pe) is used to treat spider veins and other very small varicose veins.
A small amount of liquid chemical is injected into a vein using a very fine needle. The chemical scars the inner lining of the vein, causing it to close off.
Laser surgery
This procedure applies light energy from a laser onto a varicose vein. The laser light makes the vein fade away.
Laser surgery mostly is used to treat smaller varicose veins. No cutting or injection of chemicals is involved.
Endovenous Ablation Therapy
Endovenous ablation (ab-LA-shun) therapy uses lasers or radiowaves to create heat to close off a varicose vein.
Endoscopic vein surgery
For endoscopic (en-do-SKOP-ik) vein surgery, your doctor will make a small cut in your skin near a varicose vein. He or she then uses a tiny camera at the end of a thin tube to move through the vein. A surgical device at the end of the camera is used to close the vein.
Endoscopic vein surgery usually is used only in severe cases when varicose veins are causing skin ulcers (sores). After the procedure, you usually can return to your normal activities within a few weeks.
Ambulatory phlebectomy
For ambulatory phlebectomy (fle-BEK-to-me), your doctor will make small cuts in your skin to remove small varicose veins. This procedure usually is done to remove the varicose veins closest to the surface of your skin.
vein stripping and ligation
Vein stripping and ligation typically is done only for severe cases of varicose veins. The procedure involves tying shut and removing the veins through small cuts in your skin.
You’ll be given medicine to temporarily put you to sleep so you don’t feel any pain during the procedure.
Vein stripping and ligation usually is done as an outpatient procedure. The recovery time from the procedure is about 1 to 4 weeks.
DEEP VEIN THROMBOSIS (DVT)
Deep vein thrombosis (throm-BO-sis), or DVT, is a blood clot that forms in a vein deep in the body. Blood clots occur when blood thickens and clumps together.
Most deep vein blood clots occur in the lower leg or thigh. They also can occur in other parts of the body.
A blood clot in a deep vein can break off and travel through the bloodstream. The loose clot is called an embolus (EM-bo-lus). It can travel to an artery in the lungs and block blood flow. This condition is called pulmonary embolism (PULL-mun-ary EM-bo-lizm), or PE.
PE is a very serious condition. It can damage the lungs and other organs in the body and cause death.
Blood clots in the thighs are more likely to break off and cause PE than blood clots in the lower legs or other parts of the body. Blood clots also can form in veins closer to the skin’s surface. However, these clots won’t break off and cause PE.
What Causes Deep Vein Thrombosis?
Blood clots can form in your body’s deep veins if:
- A vein’s inner lining is damaged. Injuries caused by physical, chemical, or biological factors can damage the veins. Such factors include surgery, serious injuries, inflammation, and immune responses.
- Blood flow is sluggish or slow. Lack of motion can cause sluggish or slow blood flow. This may occur after surgery, if you’re ill and in bed for a long time, or if you’re traveling for a long time.
- Your blood is thicker or more likely to clot than normal. Some inherited conditions (such as factor V Leiden) increase the risk of blood clotting. Hormone therapy or birth control pills also can increase the risk of clotting
How Is Deep Vein Thrombosis Diagnosed?
- Medical History
To learn about your medical history, your doctor may ask about:
- Your overall health
- Any prescription medicines you’re taking
- Any recent surgeries or injuries you’ve had
- Whether you’ve been treated for cancer
- Physical Exam
check the legs for signs of DVT, such as swelling or redness. also will check the blood pressure and the heart and lungs.
Diagnostic Tests
Ultrasound The most common test for diagnosing deep vein blood clots is ultrasound. This test uses sound waves to create pictures of blood flowing through the arteries and veins in the affected leg.
D dimer test A D-dimer test measures a substance in the blood that’s released when a blood clot dissolves. If the test shows high levels of the substance, you may have a deep vein blood clot. If your test results are normal and you have few risk factors, DVT isn’t likely
venography if an ultrasound doesn’t provide a clear diagnosis. For venography, dye is injected into a vein in the affected leg. The dye makes the vein visible on an x-ray image. The x ray will show whether blood flow is slow in the vein, which may suggest a blood clot.
Other tests used to diagnose DVT include magnetic resonance imaging (MRI) and computed tomography (to-MOG-rah-fee), or CT, scanning. These tests create pictures of your organs and tissues.
Treatment for DVT
The main goals of treating DVT are to:
- Stop the blood clot from getting bigger
- Prevent the blood clot from breaking off and moving to your lungs
- Reduce your chance of having another blood clot
ANTICOAGULANTS Anticoagulants (AN-te-ko-AG-u-lants) are the most common medicines for treating DVT. They’re also known as blood thinners.
These medicines decrease your blood’s ability to clot. They also stop existing blood clots from getting bigger. However, blood thinners can’t break up blood clots that have already formed. (The body dissolves most blood clots with time.)
Blood thinners can be taken as a pill, an injection under the skin, or through a needle or tube inserted into a vein (called intravenous, or IV, injection).
Warfarin and heparin are two blood thinners used to treat DVT. Warfarin is given in pill form. (Coumadin® is a common brand name for warfarin.) Heparin is given as an injection or through an IV tube.
THROMBIN INHIBITORS These medicines interfere with the blood clotting process. They’re used to treat blood clots in patients who can’t take heparin.
THROBOLYTICS quickly dissolve large blood clots that cause severe symptoms. Because thrombolytics can cause sudden bleeding, they’re used only in life-threatening situations.